The Future of Medicaid in Utah: A KUER Special Series
Part 1: Understanding the Program
By Whittney Evans
Monday July 30, 2012
Part 2: The Spend-down
By Dan Bammes
Tuesday July 31, 2012
Part 3: Gaps in Services and Gaps in Coverage
By Terry Gildea
Wednesday August 1, 2012
Part 4: We Are All Affected
By Andrea Smardon
Thursday August 2, 2012
Part 1: Understanding the Program
By Whittney Evans
Utah lawmakers are faced with a big decision: to expand or not to expand the Medicaid program. But what do we know about the program? What do people in Utah think they know about the program? And what is life like for those getting help from the program have been transformed by Medicaid? In part one of our series The Future of Medicaid in Utah, we set out to answer these and other important questions.
“Older people, freebies, handout’s,” says Salt Lake City resident Jeff Steal.
But Steal might have a bit of a simplistic view of the program.
First, to be clear, Medicare is a federal program designed to serve the healthcare needs of senior citizens.
Medicaid on the other hand is a federal state partnership that was created to help those in need who didn’t have access to health insurance. But it’s grown to serve other populations.
There are more than 250,000 people on Medicaid today in Utah, about two thirds of them are children. The program also serves pregnant women, about 2,400 elderly people in nursing homes, people with disabilities and low-income adults with children.
“I’m not sure that I really agree with it being for the younger people,” Lehi resident David Tigner says. “I think they should probably get their own insurance or get a job and get insurance.”
Currently Medicaid doesn’t cover adults without children, but that could change if the program were expanded under the guidelines outlined in the Affordable Care Act. The expansion could mean 50,000 more Utahn’s would be eligible for Medicaid.
18-year-old year old Arthur Morris is an example of a young adult who can neither work nor purchase private insurance. He was born with a hole in his heart and had open heart surgery at just five months old. His mother, Margene Morris, says when he didn’t reach any milestones, like walking or crawling some genetic tests determined he had a rare chromosome disorder.
“He has severe speech delay, motor skill delay, sleep disorder,” Morris says. “He can have violent outbursts and he has mental retardation and recently he’s been diagnosed with autism spectrum disorder. So he’s been quite a challenge.”
The Morris family has been involved in the Neuro-behavior Home Program at the University and Utah for about eight years. They only have access to the program because Arthur is eligible for Medicaid. Here, Morris says Arthur has a team of specialists working on his behalf in ways that his pediatrician alone could not.
“He’s very violent and can have some real challenging behaviors,” Morris says. “So it’s been a world of difference to have a team of doctors who are familiar with what he’s dealing with.”
Although Arthur is not allowed to have personal funds of his own, the program didn’t take the Morris’ income into consideration.
“We didn’t have to be poor and broke, even though we were probably there, but no, they didn’t even consider that,” she says.
Nearly all private insurers’ exclude coverage from those diagnosed with autism or other mental disabilities. Morris says without Medicaid, her family would be paying more than $2000 a month out of pocket for Arthur’s Medication.
“We couldn’t have had any of the things that have made Arthur’s life so much better without Medicaid,” she says. “We couldn’t have afforded it. He probably wouldn’t be alive today.”
Arthur is an example of someone who will probably receive Medicaid indefinitely. But not everyone who benefits from the program requires that kind of long-term care.
Back in Salt Lake City, resident Tony Pruitt says Medicaid was originally designed to provide temporary help for those who are struggling.
“But it’s unfortunately become a permanent situation for a lot of people and therefor gets abused,” Pruitt says. “So it’s kind of sad and frustrating because it enables people to continue bad habits, instead of do something with their life.”
35-year-old Clarissa Blackmer exemplifies what Pruitt considers the original intent of the program.

Medicaid gave her the short-term support she needed to eventually become self-sufficient. Blackmer had a series of medical issues manifest shortly after moving to Utah in her twenty’s to go to college. She suffers from fibromyalgia, rheumatoid arthritis and two heart conditions. On top of that, her sodium and potassium levels drop suddenly and randomly causing her to faint. While in school Blackmer capped out on her parents insurance after only a handful of trips to the hospital and was forced to drop out of school.
“I needed to have some stable medication,” Blackmer says. “I needed to constantly be seeing specialists and have the right specialists and for that I needed insurance. That was the only way I could physically be able to not be bedridden.”
With the help of Medicaid, Blackmer was able to finish school. And she did it quickly, receiving her bachelor’s degree in two years instead of four. She’s now a social worker for the state of Utah, working with people who are on Medicaid.
“I just am bound and determined to work despite the medical conditions,” she says. “I would rather be an example to others than just live off of the system.”
Blackmer says she’s nervous about the stigma surrounding the program.
“I work with families who desperately need it,” she says. “It will provide stability. It will keep kids in their homes rather than having to go into a system.”
Judy Hillman, Executive Director of Utah Health Policy Project, advocates for more access to affordable care.
“Anyone you go out to, an adult under 133 percent of the poverty [level] and you ask them, do you want to get into a job and into a place in your life where you can earn more money and therefore also be in private insurance and the answer is always yes,” she says.
But Hillman says they’re not going to get there without descent coverage. She says Medicaid is really a tool for them to get on and stay on that path to self-sufficiency.
Utah lawmakers have yet to make a decision on whether or not to expand Medicaid and offer coverage to a population that is currently uninsured. The federal government has pledged to cover 100 percent of the cost of that expansion for the first three years and after that they will pay up to 90 percent of the cost. State lawmakers expect to make that decision in the next Legislative Session.
Part 2: The Spend-down
By Dan Bammes

Utah lawmakers will decide in their next legislative session whether or not to expand Medicaid under the guidelines outlined in the Affordable Care Act. Unlike Medicare, which is a federal program for the elderly, Medicaid is a partnership with states that provides a healthcare safety net for those in need.
But qualifying for Medicaid is not automatic. The income and eligibility requirements are complex and the state employs dozens of people to help make those determinations.
On a typical morning inside a brown brick office building near the Salt Lake City airport, dozens of staffers in the Utah Department of Workforce Services call center are talking to people applying for the many different Medicaid programs. Some are for pregnant mothers. Others are for people who need nursing home care, or for women who discover they have breast cancer after a routine screening.
About 34-percent of the people who apply are turned down for one reason or another, but call center manager Melissa Presley says that’s not their goal.
“We want to help people,” Presley tells KUER. “We want to get people services and we want to make sure people are taken care of. These staff out here don’t do these things for the money. They do it to help people. They have good hearts and they want to help people.”
It’s not always families in poverty who need the help. Sometimes, It’s those who’ve had catastrophic health problems or who’ve exceeded the lifetime coverage limits of their private insurance.
Bobbi Mathews lives in a large home in West Jordan, but it seems empty without her daughter Katie, who passed away two years ago at the age of 15. For most of her life, Katie needed round-the-clock care.

“She was born with DiGeorge Syndrome,” Bobbi explains. “She had a lot of costs. She had surgeries, home health, a lot of prescriptions, things like that. And when she reached the age of 9, she reached her cap on her medical insurance, which was two-and-a-half million. So then we were forced to seek other options.”
Those options included borrowing against their home and running up thousands of dollars in debt while they waited to qualify for a Medicaid program for children who depend on technologies such as oxygen to survive.
“They were really nice,” Bobbi says of the Medicaid eligibility workers. “They just said they were full and didn’t have an opening at the time. When they had one, [they] would just give us a call. In the meantime, were just scrambling to pay what we could ourselves. And then, after that two-year waiting period, there was an opening. And usually, it was because another child had passed away, which you don’t like to think about.
The Affordable Care Act eliminates the lifetime maximums on private health insurance. If the law had been in effect during Katie’s lifetime, the Mathews wouldn’t have needed any help from Medicaid. As it is, they’ll be paying off the money they borrowed for many years to come.
Other families make sacrifices just to qualify for Medicaid when their needs aren’t covered by private insurance.
Tammy and Dallyn Zundel of Orem have a daughter with another rare genetic disorder, eosinophilic gastroenteritis. Their private insurance refused to cover a special amino acid formula that is the only food Ashley can eat that doesn’t make her horribly sick. It costs about $1400 a month.
“Our church stepped in,” Tammy says, “and neighbors stepped in, even did fundraising for us, did a garage sale, did a bake sale.”
When that wasn’t enough, the Zundels sought help from Medicaid.
“It’s amazing, when they get the right, proper treatment,” Tammy continues, “how well their disease is managed. Which is what we weren’t getting from our insurance. We weren’t allowed to have that kind of effective, proven treatment, so we had to go find it, the coverage, elsewhere.”
That’s the good news. But the Zundels find themselves stuck in what’s called a “spend-down.” To qualify for Medicaid, they had to reduce their family income by about 20%. Her husband earns about $47,000 a year as an art instructor, supporting a family of five. The program’s income limits keep Tammy from getting a job. They have to be careful not to keep too much money in savings and they can’t have too much equity in the cars they drive. Their older children couldn’t have jobs while they were in high school without risking their family’s eligibility for Medicaid.
Grateful as she is for the help, Tammy also believes the spend-down is holding them all back.
“I don’t want to be forced to take jobs that depend on what the income is,” she says. “I feel like – my husband has a master’s degree and I’m working on a bachelor’s right now. And I would like to be able to know that we, as a family, can meet our financial potential and our personal potential without being dictated off of what eligibility is for Medicaid.”
Jason Cooke from the Utah Health Policy Project believes those spend-down requirements work against Medicaid clients who could otherwise do a better job of supporting themselves.
“Asset tests are inherently barriers to people getting into the system,” Cooke tells KUER. “When you look at the kinds of things that are asked, people have to have a car, for example, to get to work. Or don’t we want these people to work? Of course we do. They want to work for the most part. They want to be in jobs if they can find jobs.”
The Zundels might also benefit from the Affordable Care Act. It eliminates asset tests for Medicaid, and since it doesn’t allow insurance companies to deny coverage based on pre-existing conditions, it could allow them to shop around for a private insurance plan that covers the special formula Ashley needs to survive.
In addition to a decision on the expansion of Medicaid, the state of Utah is required to set minimum standards for health care coverage under the Affordable Care Act. That process is underway now in the legislature’s Health Care Reform Task Force, with a recommendation due on September 1st. Tammy Zundel has been actively lobbying to make sure those standards included the specialized diet her daughter needs. And what’s included in that basic health care plan could make a big difference in the future to the families who depend on Medicaid today.
Part 3: Gaps in Services and Gaps in Coverage
By Terry Gildea
The expansion of Medicaid as outlined in the Affordable Care Act is designed to give more people access to healthcare services. Without the expansion, a portion of the Utah’s population living on the edge of poverty may remain uninsured. But some believe that Medicaid doesn’t do enough for those who are already enrolled. In part 3 of our series, The Future of Medicaid in Utah we examine the gap in services already provided and the coverage gap that will continue to exist if Medicaid is not expanded.
One day a few years ago, Karlene Kidman didn’t feel well. She had a terrible headache and her breathing was labored. So she went the emergency room at a local hospital near her home in Layton. Karlene was worried that the pneumonia she’d had ten months before had come back. She was right.
“They said I probably needed to stay in the hospital a couple of days. And I said it doesn’t matter, PCN does not cover hospital stays at all,” said Karlene Kidman.
PCN stands for Primary Care Network, a Utah Medicaid program created in 2002. It’s designed to provide a set of health benefits to a larger pool of recipients at a lower cost to taxpayers. It covers doctor’s visits, four prescriptions a month and some trips to the emergency room, but PCN doesn’t cover hospital stays, visits with specialists other services related to catastrophic care. So Karlene was sent home from the emergency room with prescription for antibiotics. A few months later, Karlene injured her knee, but PCN wouldn’t cover a visit to a specialist or a surgery she needed. Frustrated by the limited resources of her PCN plan, she tried to explore other options.
“At that time I went to my employer and I said I really need some health insurance and so they looked up health insurance for me and my daughter and it would’ve been… the monthly premium for the insurance was more than I made a month. So there’s no way I could pay that,” Kidman said.
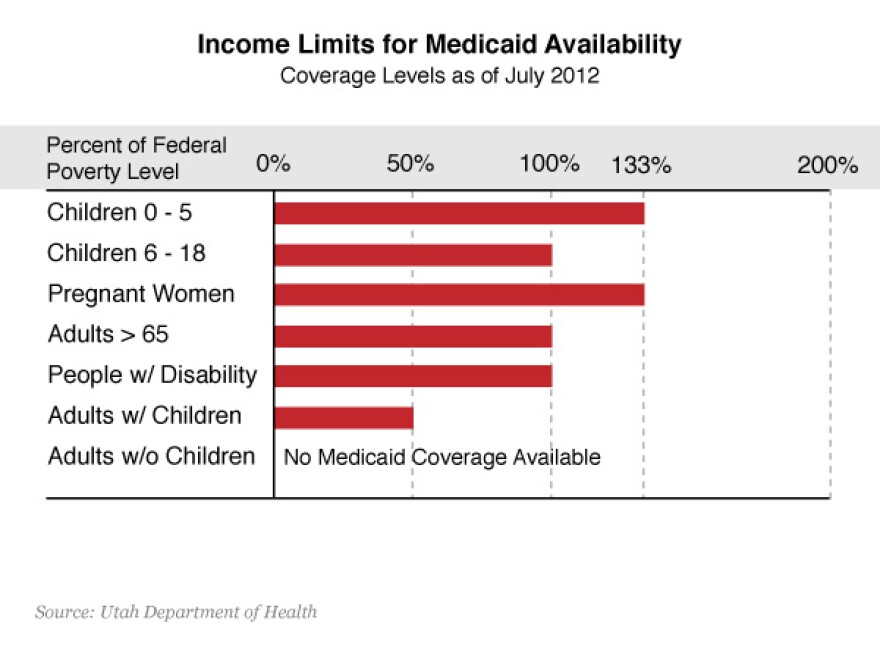
The best Karlene’s employer could do was give her a modest raise, but that raise put her over the eligibility limit for PCN and her enrollment in the Primary Care Network was discontinued. The raise from her non-profit employer wasn’t enough to afford private health insurance, so Karlene has lived without health coverage since 2007. If Medicaid is expanded, an estimated 50,000 additional Utahns could enroll. Income eligibility levels would rise significantly for adults with children, from 50 percent of the federal poverty level to 133 percent. Adults without children, a population that is currently not eligible for the program, could also enroll up to 133 percent of FPL or an annual income roughly 30,000 dollars for a family of four. Jason Cooke is the Medicaid policy analyst for the Utah Health Policy Project. He says expansion would finally provide coverage to a significant portion of the population.

“These are people who caught between poverty and having enough money to be able to buy coverage. The commercial market has never, never responded to that need sufficiently and they've had lots of opportunity. So there’s no choice other than leaving these people uninsured and having the problems that we currently have un-insurance in the healthcare system,” said Cooke.
But members of a conservative think tank in Utah believe government should not be involved in providing any healthcare coverage. Stan Rasmussen is with the Sutherland Institute. He says health care services for the working poor could be provided a system of privately funded free clinics, a concept Sutherland calls authentic charity care.
“And that would be a means by which primary care could be provided at a much lower cost to providers and a much, much lower cost to those who are recipients of it. Is that going to solve all of the problems? No. But we feel that an authentic charity care element is an essential component in a truly functional and effective approach to healthcare for people in the state of Utah,” said Rasmussen.
But the kind of charity care network that Rasmussen envisions doesn’t completely exist and an expanded Medicaid program could benefit some families sooner, like The Woodruff family in North Salt Lake. Chelsea Woodruff works from home taking airline customer service calls and gets some health insurance for herself and their two children, but her husband Kyle is currently unemployed they can’t afford to pay for his insurance.
“It was two hundred and fifty three dollars a month to cover me and the two children. It was going to be four hundred and fifty dollars a month to cover all of us and that difference we just couldn’t make up in our budget, there was no way to cover it,” Chelsea Woodruff said.

This family of four survives on $27,000 a year. That’s roughly 132 percent of the federal poverty level, which means if Medicaid was expanded tomorrow under the Affordable Care Act, Kyle would qualify for Medicaid, but he’s currently uninsured. Kyle has been blind his entire life. He doesn’t qualify for disability benefits through Medicaid because his blindness hasn’t stopped him from working. Last year he developed a skin infection called cellulitis while he was uninsured and paid out of pocket for his treatment. He continues to be concerned about a chronic health condition he has with kidney stones.
“The entire episode of cellulitis took a week, and that was it. And it was a nine hundred dollar week. If kidney stones happens, which… they’ve told us that I have four in my right and two in my left, so it’s not if, but when,” said Kyle Woodruff.
The Woodruff family wants to get into a situation where they have access to private health insurance that will cover their medical needs, but a rough economy and job market have hit the Woodruff’s hard. Chelsea was unemployed for more than two years and the health insurance that Kyle had at his job during that time, didn’t completely many of the chronic health problems she needed treatment for.
“When we got married, when we moved into this home we both had full-time jobs, it looked like everything was going to be fine and we filed bankruptcy last year to wipe out sixty-thousand dollars in medical debt because I was laid off for two and a half years while he was making minimum wage,” said Chelsea Woodruff.
Chelsea is so upset with the way the system works in Utah that she’s running for public office. She’s the Republican nominee in State Senate District 1 and will face Democrat Luz Robles in November. She’s concerned that insurance companies don’t work with consumers to disclose what the least expensive care options are, so that people don’t end up paying high prices for minor procedures.
“I should be able to control my own medical costs and make decisions for my own healthcare based on what I can afford,” Chelsea Woodruff said.
Utah lawmakers plan to decide in the next legislative session whether the state will move forward with an expansion of Medicaid or leave the program as it is. If nothing is done, gaps in services and coverage will still exist. People like Kyle Woodruff will continue to live day to day without coverage, hoping that a catastrophic healthcare crisis isn’t around the corner.
Part 4: We Are All Affected
By Andrea Smardon

After the Supreme Court decision on the Affordable Care Act, states are faced with a decision on whether to expand Medicaid eligibility. Utah remains undecided. In the last story in our series, The Future of Medicaid in Utah, we look at how the decision affects all of us as taxpayers and healthcare consumers.
Charles Pruitt is a pediatric emergency medicine physician in Salt Lake City. He’s seen his share of tragedies in the ER, but one little girl still haunts him - not just because she died under his care, but because he believes her death was preventable. She came in complaining of headaches – headaches so bad she couldn’t sleep. He asked her mother how long it had been going on. The mother told him several months.
“I did a CAT scan of the girls head, and found what I really feared the most, which was a large brain tumor, a very large brain tumor,” Pruitt said.

Pruitt had to tell the mother and girl that the tumor was inoperable, and the girl was going to die.
“In the back of my mind I kept thinking, why did she have to wait so long? I started to feel like I had failed her, and like we - as a medical community - had failed this little girl and her mother. And then my frustration turned more to anger,” said Pruitt.
The family did not have insurance, and the mother - a single parent – told him that, even working two jobs, she could not afford to take her daughter to a primary care doctor.
%22I%20was%20left%20with%20the%20feeling%20that%20this%20was%20so%20preventable%2C%20this%20tragedy.%22
“I was left with the feeling that this was so preventable, this tragedy,” said Pruitt. “Had the family, the little girl and her mother, had the options that every child should have - just the ability to go and have your symptoms checked out when they occur - that this wouldn’t have happened. This little girl would still be alive today.”
Pruitt says he’s seen more uninsured showing up in the ER since the recession. He’s in favor of expanding Medicaid in Utah, not only because it would increase access to healthcare, but because he says it would bring down the costs for those who already have insurance. It’s Pruitt’s contention that we all pay for the uninsured in the form of higher premiums. So, he says, we can pay now by funding an expansion of Medicaid or pay later as healthcare costs continue to grow.
“We would all be better off if this little girl had had access to healthcare, and overall the costs of medical care would be a little bit less,” said Pruitt.
On the other side of the spectrum is Stan Rasmussen of the Sutherland Institute, a conservative think tank in Utah.
“Only in the United States is death considered an option,” said Rasmussen, “We have allowed healthcare to get to a point, where if people get sick and actually die, that the assumption is made that somebody fouled up, and things have unfolded that shouldn’t happen.”
It’s Rasmussen’s position that government is overly involved in healthcare, and that an expansion of Medicaid is a move in the wrong direction.
“We believe that the expansion would make more Utahns dependent on a government program that’s already becoming unaffordable,” said Rasmussen, “Lawmakers should stand up and refuse to sell Utahns self-reliance and independence for a few dollars.”
%22We%20believe%20that%20the%20expansion%20would%20make%20more%20Utahns%20dependent%20on%20a%20government%20program%20that%27s%20already%20becoming%20unaffordable.%22
State lawmakers are now weighing the arguments. Currently the federal government pays for 70 percent of Utah’s Medicaid funding. Under the Affordable Care Act, the federal government would foot 100 percent of the funding for Utah’s Medicaid expansion for the first three years, gradually decreasing to 90 percent by 2020. Representative James Dunnigan is Chair of the state’s Health System Reform Task Force. He says even with substantial federal contributions, he’s concerned about how much money Medicaid will eventually cost the state.
“We need to decide… do we want to do it, can we afford to do it? Even though the federal government picks up 100 percent over the first several years, our share increases, and we’re talking a lot of dollars.
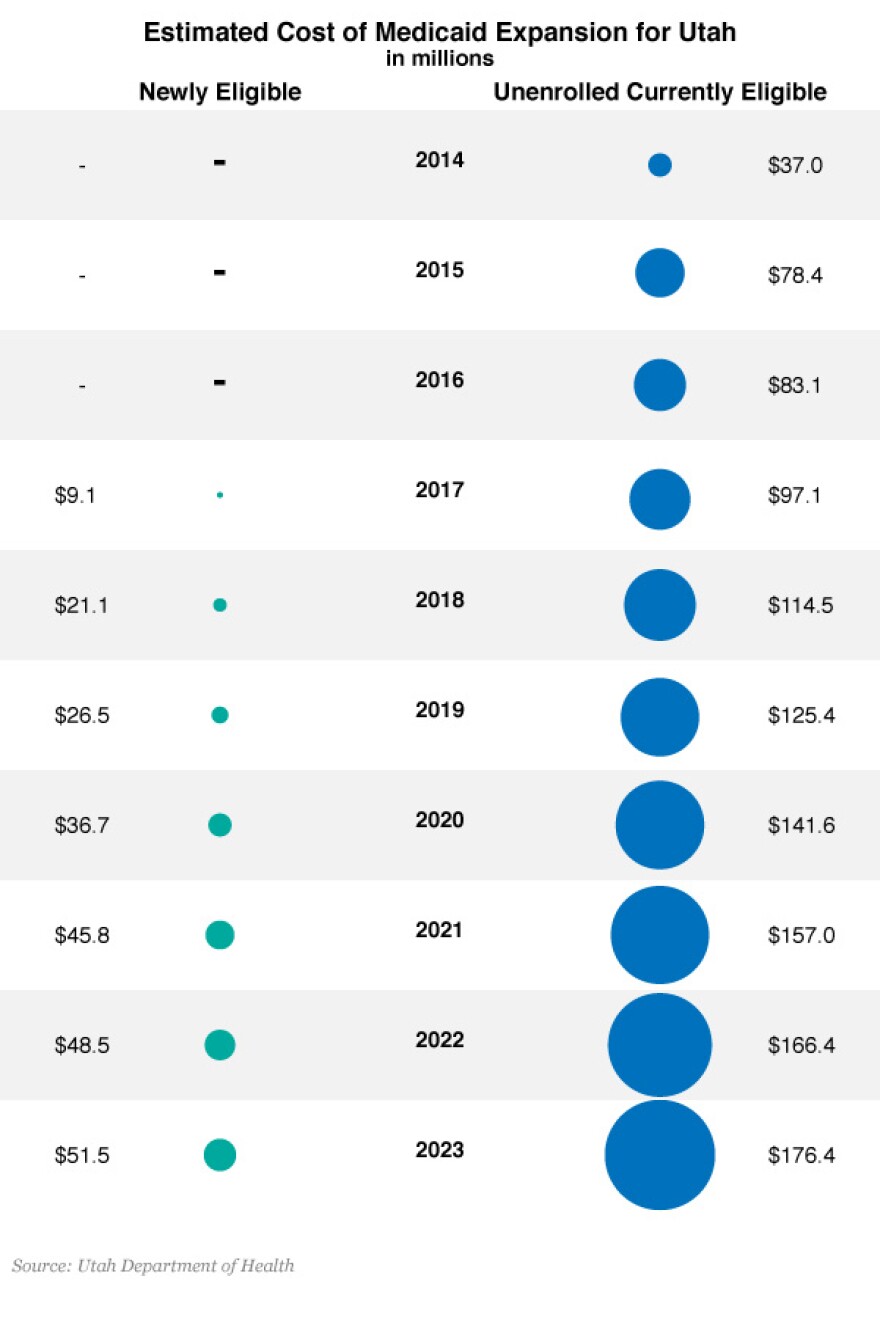
The state Department of Health has estimated that if Utah expands Medicaid eligibility up to 133 percent of the poverty level, it would cost the state 239 million dollars over the next 10 years. It would cost the federal government more than 3.5 billion. Those figures don’t take into account those already eligible for Medicaid who are expected to enroll when the individual mandate goes into effect. Utah would be responsible for paying for 30 percent of those costs – which would amount to more than 900 million dollars in the next decade. Senator Stuart Adams is on the Task Force, and he says the growth of Medicaid is unsustainable.
“Nobody’s figured out how to pay for it,” said Adams, “If we have to borrow, or we have to print money, or some other unsustainable way, someone is not being realistic with the promises or the commitment they’re making to the public.”
But even with these concerns, Utah’s Governor and lawmakers aren’t saying no outright to a Medicaid expansion. Norman Thurston is the state’s Health Reform Implementation Coordinator. He says the US Department of Health and Human Services still hasn’t provided some important information that may inform Utah’s decision.
“There is a big question that’s unanswered in my mind, and I think a lot of states have now brought this up, which is… what alternatives do we really have? Because it looks on paper like it’s black and white -you either have the expansion or you don’t - but we’re pretty sure that’s not the end of the story,” Thurston said at a meeting of the state’s Health System Reform Task Force.
Thurston wants to know if there is room for a partial expansion, waivers, or block grants. HHS officials would not tell KUER whether the federal government will negotiate on this point. Without this information, Thurston says it’s too soon to make a decision.
The Department of Health estimates that more than 50,000 additional people could enroll in Medicaid if the state expands eligibility. If the state chooses not to expand, it’s not clear what option these people will have for health insurance, or whose responsibility it would be to help them… if anyone.
